PayerIQ™
PayerIQ™
PayerIQ™ AI-Powered Payer Intelligence, Contract Analytics & Underpayment Recovery Platform
Built for Medical & Dental Organizations and Independent practices. No more with the small practice not have visibility into to thier agreements and allowable, and now DSO and MSO can have a cohesive review of thier agreement and how they are getting paid.
Most dental and medical organizations do not truly know how their payers are performing until revenue has already been lost. Payer contracts, reimbursement methodologies, fee schedules, payer policies, network agreements, underpayments, and denial trends are often buried inside disconnected systems, spreadsheets, and manual reporting processes, making it difficult to identify financial risk in real time.
PayerIQ™ changes that!
Developed by RevTech Partners, PayerIQ™ is an AI-powered payer intelligence and reimbursement analytics platform designed to help dental and medical organizations and practices identify payer performance issues, detect underpayments, monitor contractual compliance, and strengthen payer negotiation strategies across the enterprise.
Do you struggle with understanding how your payers or leases pay? Do you feel like you are working more and making less? When you come to the negotiation table, do you know your data and analytics as well as the payers do?
PayerIQ™ resolves those barriers by providing dental and medical practices and organizations with the intelligence, visibility, and analytics needed to ensure they are reimbursed in accordance with their payer agreements and contractual terms.
For too long, medical and dental organizations have operated without the same level of data, transparency, and negotiation power as the payers.
That changes now.
PayerIQ™ empowers organizations to stop operating reactively and start making strategic, data-driven decisions around:
- Payer participation
- Network agreements
- Reimbursement models
- Fee schedules
- Contract negotiations
- Lease and provider expansion strategies
- Enterprise payer performance
No longer do payers hold all the leverage. With real-time reimbursement analytics, underpayment intelligence, payer performance visibility, and AI-powered contract monitoring, practices now have the tools to protect revenue, strengthen negotiations, improve profitability, and decide which payer relationships truly align with their business goals.
It’s time for healthcare organizations to come to the table playing by the same rules — with the same level of intelligence, strategy, and financial visibility as the payers themselves.
Why PayerIQ™
Most organizations rely on delayed reporting, manual audits, and reactive analysis to identify payer issues.
By the time underpayments, denial trends, reimbursement inconsistencies, or payer compliance problems are discovered, organizations have already lost significant revenue.
PayerIQ™ delivers real-time AI-powered visibility into:
- Payer reimbursement behavior
- Contract compliance
- Network performance
- Fee schedules
- Allowables
- Underpayments
- Denial trends
- Payer risk patterns
- Reimbursement inconsistencies
- Contract performance analytics
allowing organizations to proactively protect revenue and improve payer accountability.
Benefits of PayerIQ™
PayerIQ™ combines:
- Artificial Intelligence (AI)
- Predictive Analytics
- Real-Time CARC and RARC Monitoring
- Workflow Automation
- Operational Intelligence
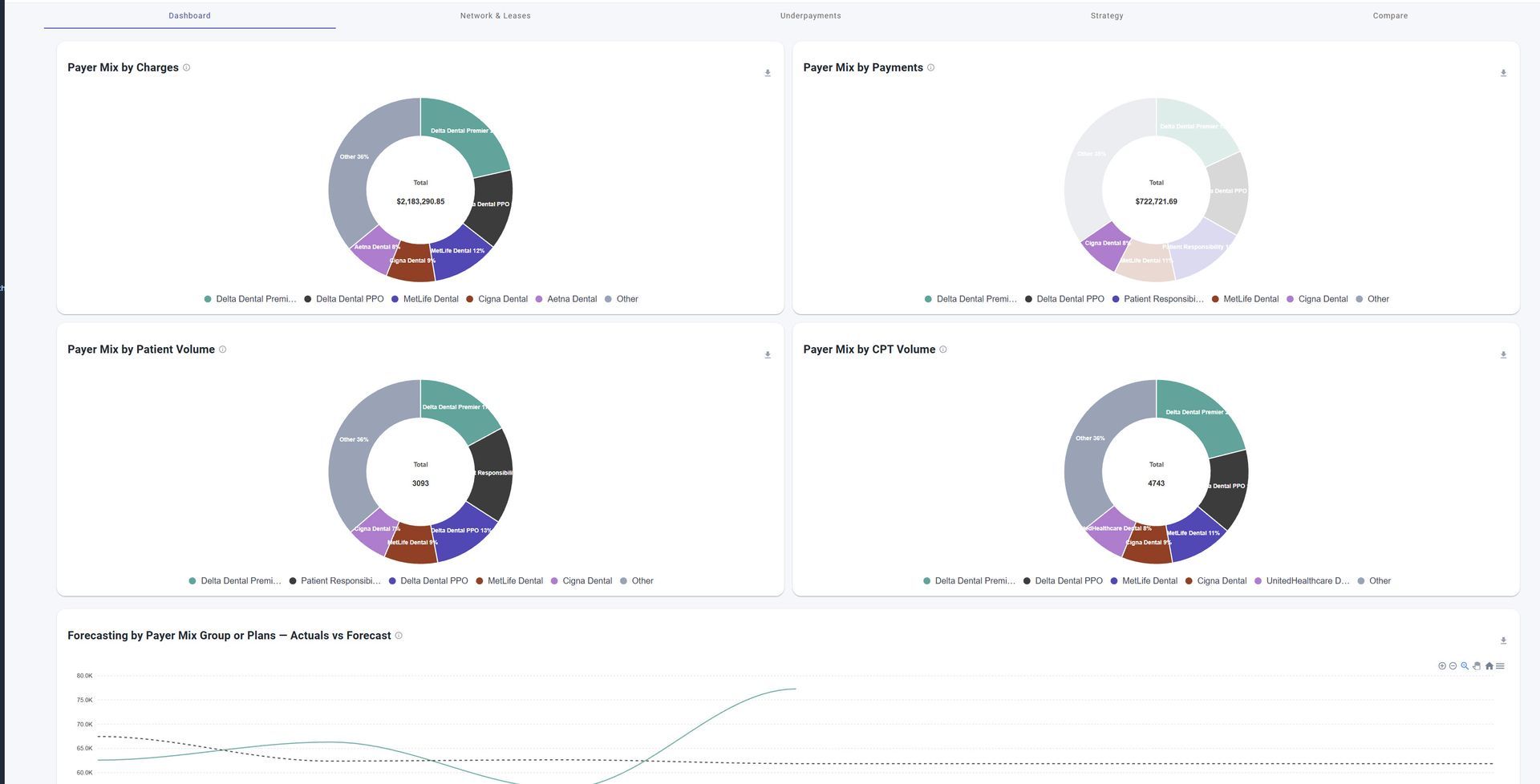
- Accelerated Financial Visibility
- Financial Performance Dashboards
- Enhanced Forecasting
- Increase Practice and Provider Transparency
- Payer Reimbursement Behavior
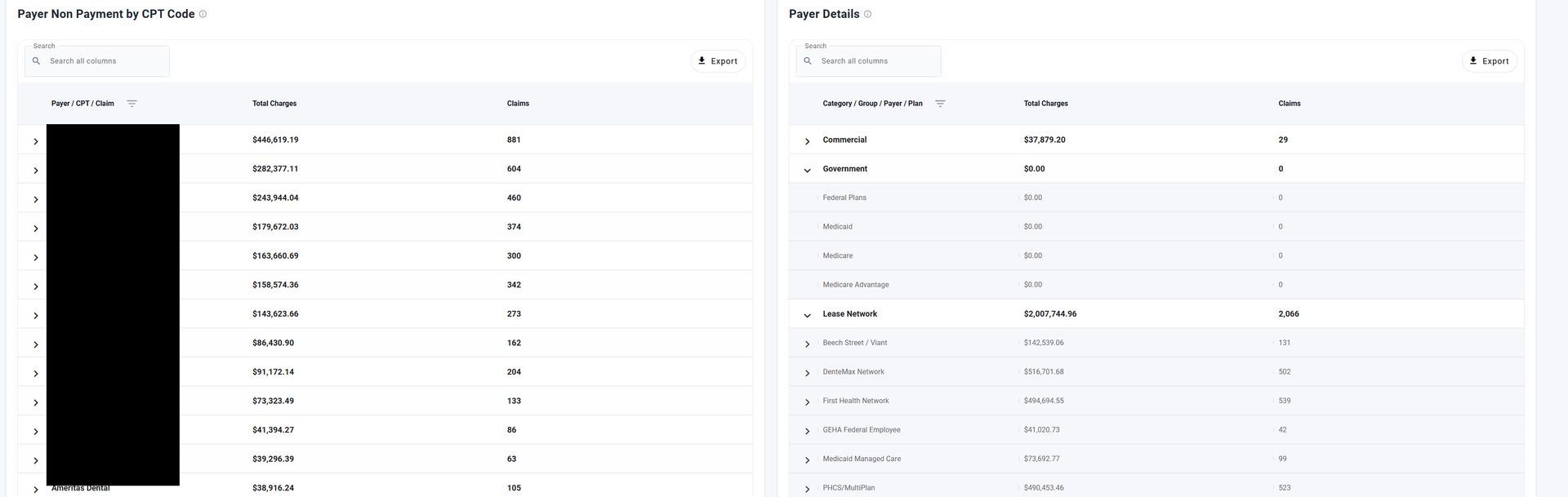
- Network/ Lease Performance
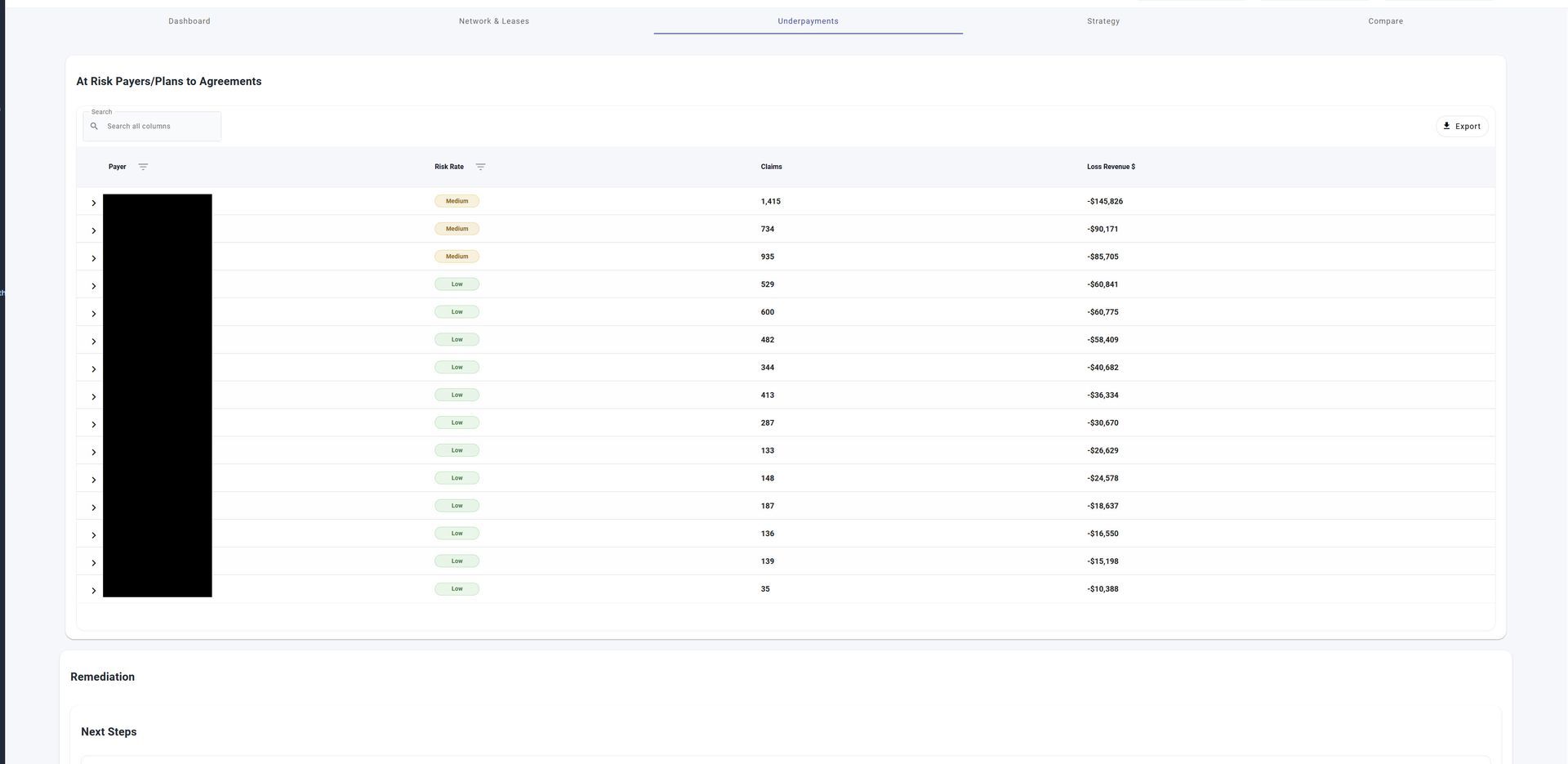
- Underpayments
To create a next-generation healthcare technology platform focused on maximizing revenue and reducing operational friction.
Key Features PayerIQ™
AI-Powered Payer Intelligence
PayerIQ™ uses Artificial Intelligence and advanced reimbursement analytics to help organizations gain visibility into payer performance, reimbursement trends, contract alignment, and financial risk across the revenue cycle. Payer behavior provides real-time financial intelligence and actionable insights.
The platform helps identify:
- Reimbursement inconsistencies
- Underpayment opportunities
- and More
Built Around Your Organization
PayerIQ™ is designed to support organizations of every size — from single-provider practices to large enterprise healthcare organizations.
The platform is structured to provide visibility across:
- Provider groups
- Organizational structures
- Payer relationships
- Network participation
- Reimbursement performance
- Enterprise financial analytics
allowing leadership teams to monitor payer activity and financial performance at both the practice and enterprise level.
Smarter Financial Visibility
PayerIQ™ provides organizations with real-time payer analytics and reimbursement intelligence designed to help teams identify financial opportunities faster and respond proactively.
The platform helps organizations:
- Improve reimbursement visibility
- Reduce revenue leakage
- Strengthen financial oversight
- Support payer strategy decisions
PayerIQ™ transforms payer management into a proactive, AI-driven financial intelligence strategy that improves visibility, strengthens financial performance, and supports smarter organizational decision-making.
From Reactive Payer Management to AI-Powered Financial Intelligence
PayerIQ™ transforms payer management into a proactive AI-driven financial intelligence strategy designed to maximize reimbursement, strengthen negotiations, and protect revenue.
Increased Visibility into Reimbursements
Increase Ability to Monitor Trends
Hold Payers Accountable To Agreements
Build Payer Strategy on Real Data
Identify Underpayments
Identify Revenue Leakage
Built for Modern Healthcare Organizations
- Dental Service Organizations (DSOs)
- Independent Dental Practices
- Medical Service Organizations (MSOs)
- Independent Medical Practices
- Multi-Site Healthcare Groups
- Hospitals & ASC
- B2B Clients
PayerIQ™ empowers organizations to move from reactive revenue management to proactive financial intelligence.
Stop Chasing Denials. Start Preventing Them.
Schedule A Demo Today
Discover how ReconIQ™ can help your organization improve cash flow, reduce denials, automate workflows, and unlock hidden revenue opportunities with AI-driven operational intelligence.
Strategic Partnerships
RevTech partners with best-in-class companies to deliver the complete technology stack for dental organizations.
National Data Solutions
Data platform, intelligence layer, managed IT, and practice integration. We turn fragmented data into actionable wisdom.
- DataVault - data governance & warehousing
- Exocomps - location-deployed ETL agents
- InsightFlow & Power BI - 72+ visualizations
- Managed IT - NIST RMF, HIPAA compliance
- Practice Integration - acquisition readiness
- AI Agents - predictive analytics & automation
Xentrios
Next-generation dental PMS built for the modern DSO. AI-enabled to lessen the administrative burden on clinical staff - informing and orienting instead of making hidden decisions. Ships with the full RevTech suite integrated out of the box.
- Cloud-native dental PMS for multi-location DSOs
- AI workforce support - reduces admin burden on clinical staff
- Transparent AI - informs and orients, never hides decisions
- Full RevTech suite integrated out of the box
- Native NDS DataVault integration
- Open API for third-party integrations
MaximizeRCM Consulting
MaximizeRCM Consulting was created to help healthcare organizations, DSOs, MSOs, and specialty practices improve operational performance, reduce denials, strengthen cash flow, and uncover revenue opportunities through real-world Revenue Cycle Management expertise.
- • Revenue Cycle Assessments & Operational Reviews
- Denial Management & Root Cause Analysis
- Revenue Leakage & Underpayment Identification
- Workflow Optimization & Process Improvement
- KPI Reporting, Dashboards & Operational Visibility
- Staff Education, RCM Training & Leadership Support