ClaimVision™
ClaimVision™
AI-Powered Claims Intelligence & Denial Prevention Platform
For Medical, Dental, DSO, MSO, and Healthcare Organizations
Most organizations don’t have a claims problem; they have a visibility problem.
By the time denials are identified, revenue has already been delayed, workflows disrupted, staff overloaded, and cash flow impacted.
ClaimVision™ changes that.
Built by RevTech Partners, ClaimVision™ is an AI-driven claims intelligence and denial prevention platform designed to provide real-time visibility into claim performance, payer behavior, reimbursement trends, and revenue leakage across the entire revenue cycle.
Built by experts with deep knowledge of CARC codes, RARC codes, payer policies, coding compliance, reimbursement logic, documentation requirements, claim editing workflows, and denial management strategies, ClaimVision™ was designed to solve the problems traditional claim scrubbers miss.
Most claim systems only verify whether a claim can be submitted.
ClaimVision™ is engineered to determine whether a claim is likely to get paid.
This is not simply about checking if every box is completed, if attachments are present, or if X-rays and narratives are connected. ClaimVision™ goes far beyond traditional claim scrubbing by using an intelligent AI-driven rules engine that analyzes:
- Payer-specific requirements
- Historical denial trends
- Coding inconsistencies
- Documentation gaps
- Modifier usage
- Authorization requirements
- Frequency limitations
- Reimbursement patterns
- Compliance risks
- Operational workflow issues before the claim is ever sent to the payer.
Do you struggle with denials based on medical necessity, bundling, downcoding, or documentation, or do you need additional documentation?
ClaimVision™ resolves those before they are sent to the payer.
Why ClaimVision™
Most denials do not happen because a claim was simply missing information. They happen because organizations lack visibility into payer rules, coding logic, documentation requirements, reimbursement patterns, operational workflows, and denial risk before the claim is submitted.
Revenue leakage often begins long before the denial is received, inside coding workflows, payer policy changes, authorization gaps, modifier usage, documentation inconsistencies, compliance risks, claim edit logic, and operational inefficiencies.
Traditional claim scrubbers only validate whether a claim can be submitted.
ClaimVision™ is designed to predict whether the claim will get paid.
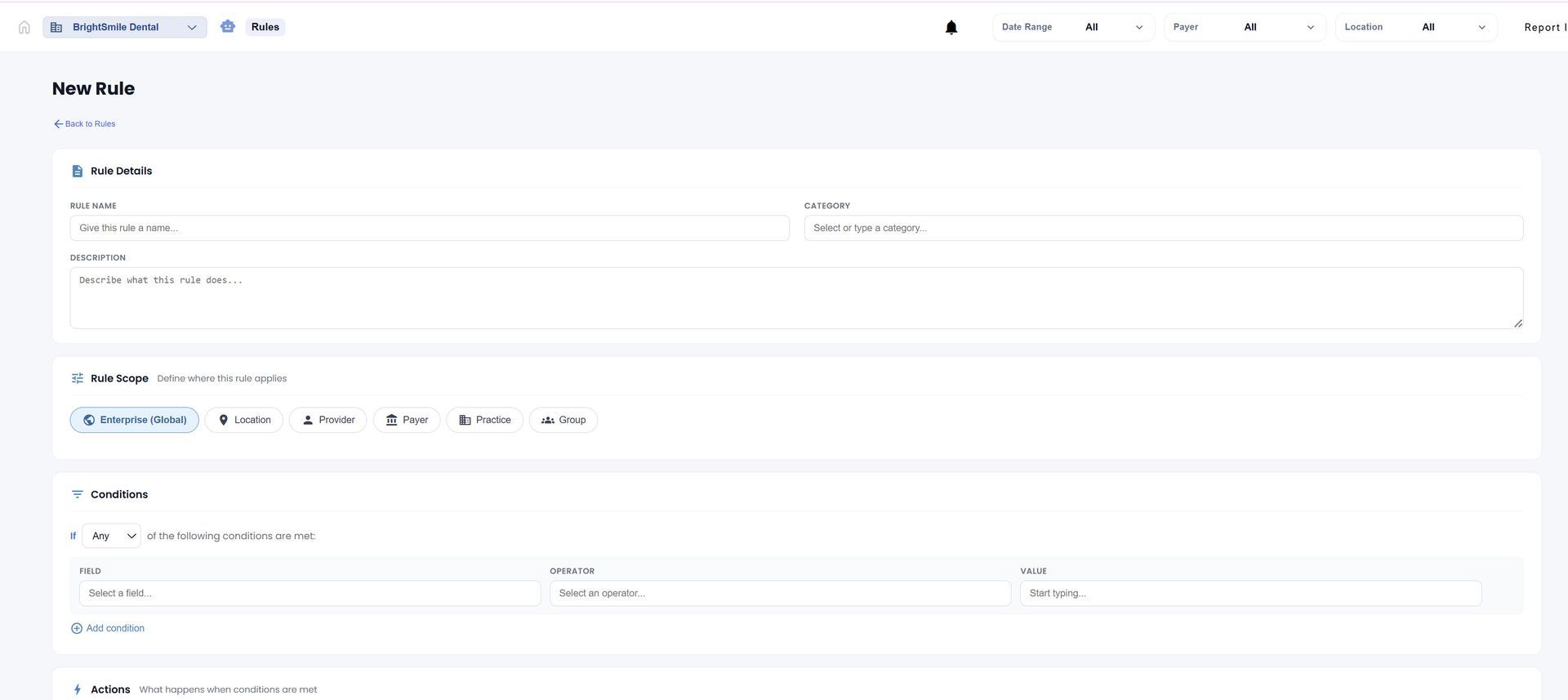
ClaimVision™ uses AI-powered claims intelligence, predictive denial analytics, payer logic monitoring, and customizable rules engines to proactively identify high-risk claims before they ever reach the payer.:
- CARC & RARC trends
- Payer-specific requirements
- Coding compliance
- Modifier logic
- Authorization rules
- Documentation gaps
- Historical denial patterns
- Reimbursement behavior
- Workflow inefficiencies
- Revenue leakage risks
Benifits of ClaimVision™
ClaimVision™ combines:
- Artificial Intelligence (AI)
- Predictive Analytics
- Real-Time CARC and RARC Monitoring
- Workflow Automation
- Operational Intelligence
- Denial Prevention Technology
- Financial Performance Dashboards
- Claims Intelligence
- Payer Analytics and Policies
- Practice Management Integration
To create a next-generation healthcare technology platform focused on maximizing revenue and reducing operational friction.
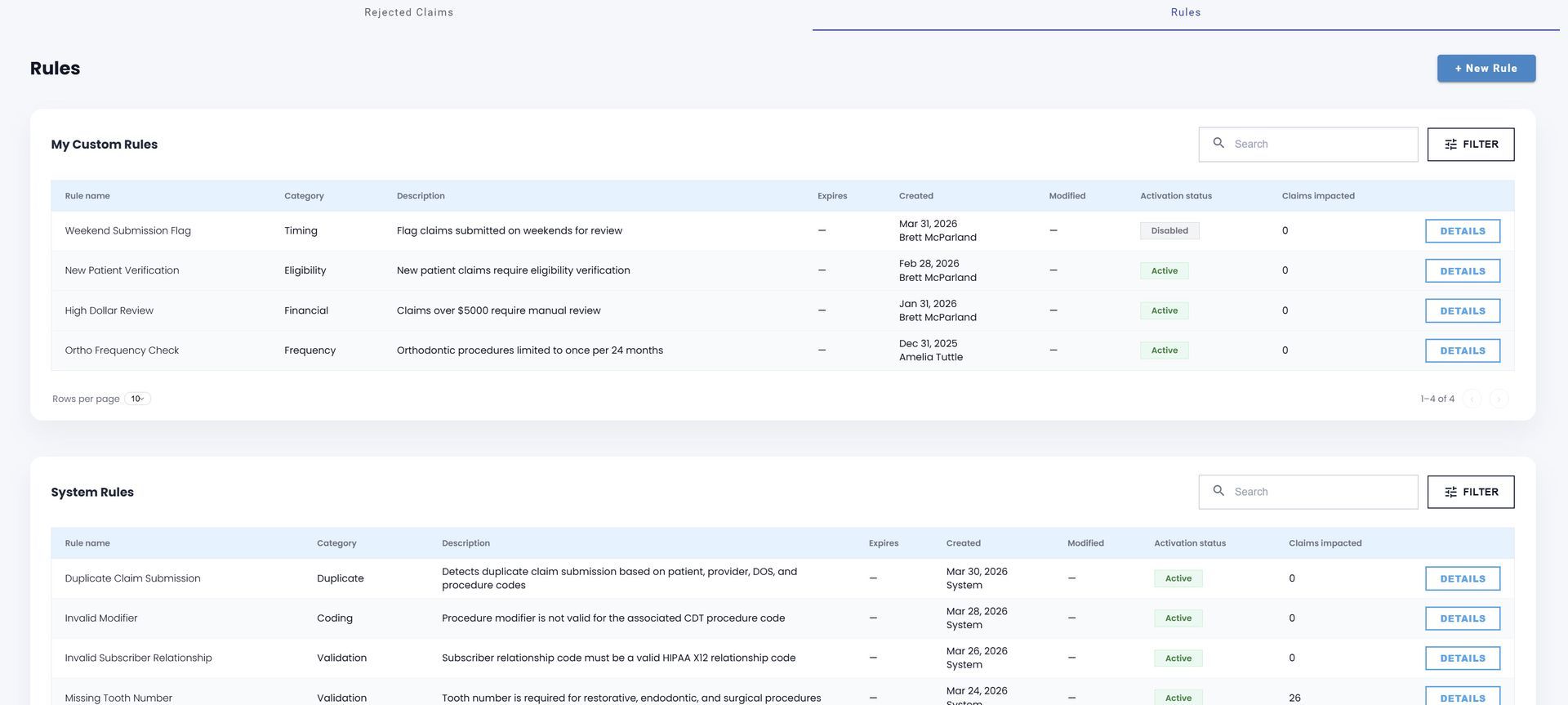
Key Features ClaimVision™
Predictive Denial Prevention
Identify claims likely to deny before submission using AI-powered payer and claims analytics.
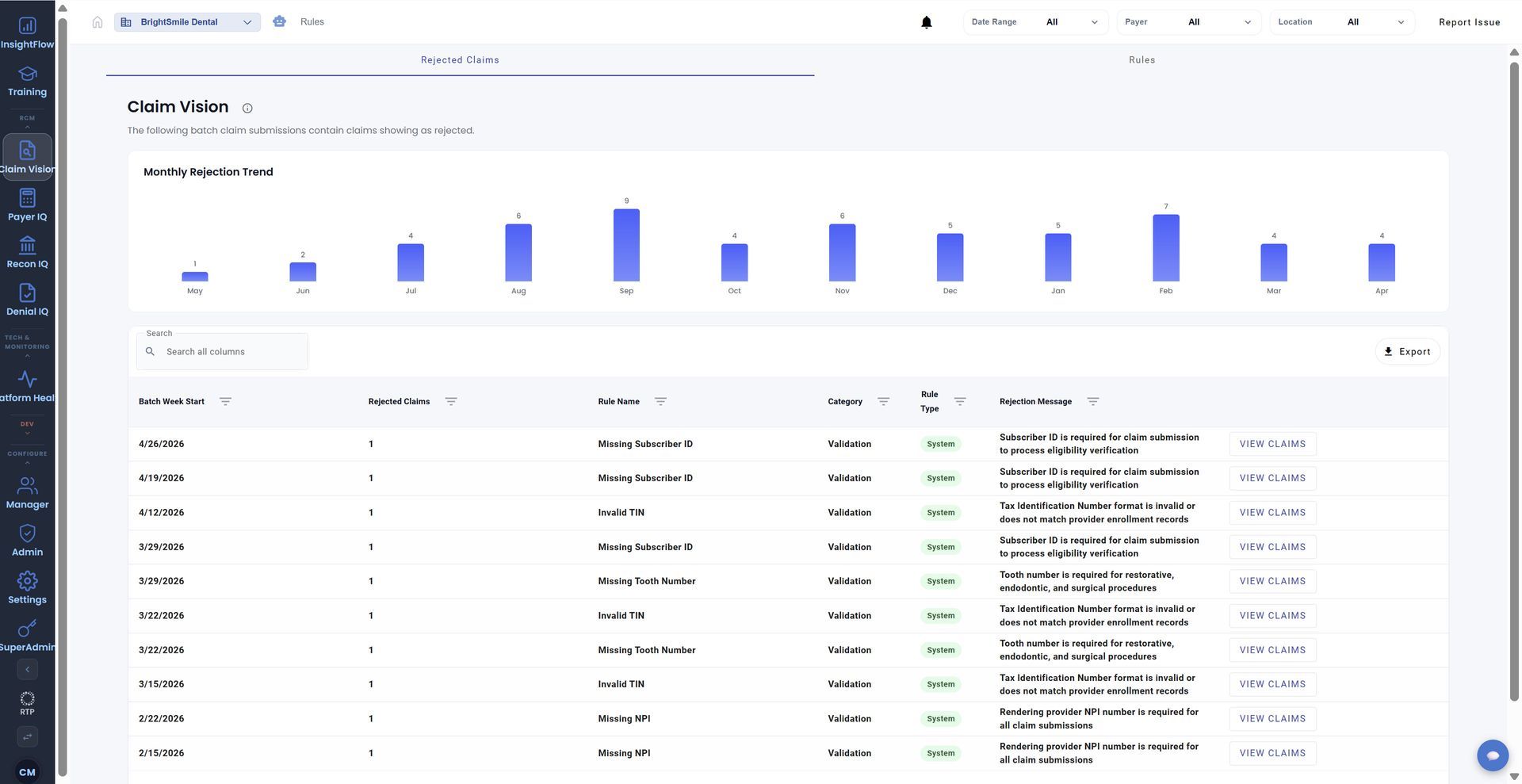
Real-Time Claims Visibility
Monitor:
- Claims Status
- Denials
- Rejections
- Appeals
- Underpayments
- Aging AR
- Payer Delays
- Workflow Bottlenecks
In real time across the organization.
Revenue Leakage Detection
Identify hidden financial loss caused by:
- Coding inconsistencies
- Documentation gaps
- Authorization failures
- Payer inconsistencies
- Workflow inefficiencies
- Missed claim opportunities
Intelligent Workflow Automation
Automate repetitive claims management tasks, including:
- Work queue prioritization
- Follow-up workflows
- Appeal routing
- Exception management
- Task automation
- Claims tracking
Executive Financial Dashboards
Turn claims data into actionable business intelligence with customizable operational and financial dashboards.
From Reactive Billing to Predictive Revenue Protection
Most organizations operate reactively — fixing denials after reimbursement delays occur.
ClaimVision™ changes the model by delivering proactive AI-driven claims intelligence designed to:
Reduce Preventable Denials
Improve the Over-the-Counter Collections
Accelerate Cash Flow
Improve Coding Accuracy
Reduce Documentation Errors
Strengthen Compliance
Reduce Manual Rework - AR Follow Up
Improve Operational Efficiency
Protect Revenue before it is Lost
Built for Modern Healthcare Organizations
- Dental Service Organizations (DSOs)
- Independent Dental Practices
- Medical Service Organizations (MSOs)
- Independent Medical Practices
- Multi-Site Healthcare Groups
- Hospitals & ASC
- B2B Clients
ClaimVision™ empowers organizations to move from reactive revenue management to proactive financial intelligence.
Stop Chasing Denials. Start Preventing Them.
Schedule A Demo Today
Discover how ClaimVision™ can help your organization improve cash flow, reduce denials, automate workflows, and unlock hidden revenue opportunities with AI-driven operational intelligence.
Strategic Partnerships
RevTech partners with best-in-class companies to deliver the complete technology stack for dental organizations.
National Data Solutions
Data platform, intelligence layer, managed IT, and practice integration. We turn fragmented data into actionable wisdom.
- DataVault - data governance & warehousing
- Exocomps - location-deployed ETL agents
- InsightFlow & Power BI - 72+ visualizations
- Managed IT - NIST RMF, HIPAA compliance
- Practice Integration - acquisition readiness
- AI Agents - predictive analytics & automation
Xentrios
Next-generation dental PMS built for the modern DSO. AI-enabled to lessen the administrative burden on clinical staff - informing and orienting instead of making hidden decisions. Ships with the full RevTech suite integrated out of the box.
- Cloud-native dental PMS for multi-location DSOs
- AI workforce support - reduces admin burden on clinical staff
- Transparent AI - informs and orients, never hides decisions
- Full RevTech suite integrated out of the box
- Native NDS DataVault integration
- Open API for third-party integrations
MaximizeRCM Consulting
MaximizeRCM Consulting was created to help healthcare organizations, DSOs, MSOs, and specialty practices improve operational performance, reduce denials, strengthen cash flow, and uncover revenue opportunities through real-world Revenue Cycle Management expertise.
- • Revenue Cycle Assessments & Operational Reviews
- Denial Management & Root Cause Analysis
- Revenue Leakage & Underpayment Identification
- Workflow Optimization & Process Improvement
- KPI Reporting, Dashboards & Operational Visibility
- Staff Education, RCM Training & Leadership Support